CDS caregivers who take care of elderly people who have osteoporosis need to know care techniques that will prevent injury to these delicate patients.
Much of the care for these individuals is the same as any other elderly person, but there are some considerations that need to be made to prevent injury to these individuals and to keep them from falling.
If you have been wanting to learn more about the kind of care that is needed for elderly people with osteoporosis, you should read on for more information. These details are important for the overall care practices that will keep these elderly people safe while they are under your care.

Primary Osteoporosis vs Secondary Osteoporosis
Osteoporosis is a joint disease that leads to joint pain, bone weakness, pain and tenderness, and also general joint and bone tenderness. This is a common disease in the elderly as a result of age and other conditions. Degenerative joint disease is a different concern than osteoporosis. Both diseases are progressive, however.
Primary Osteoporosis
Primary osteoporosis develops due to age and wear and tear of joints. The joint leads to progressive disease that damages the cushioning inside of joints as well as cartilage and overall bone strength. This is not related to injury and is related to the loss of protein content inside the bones.
This disease process is most common in those over 55. There can be other reasons that individuals might end up with primary osteoporosis as well. You can have lifelong conditions such as a lack of bone density since childhood, or you might have other disease processes that are causing your lack of healthy bone tissue.
Women can fall prey to primary osteoporosis after menopause as their hormones shift and change in response to age and the after-effects of childbirth and breastfeeding. Women naturally have less bone density than men, and this condition can lead to serious issues for overall bone health in women.
· Occurs to Women After Menopause
· Men later in Life
· Lack of optimal bone mass as a child
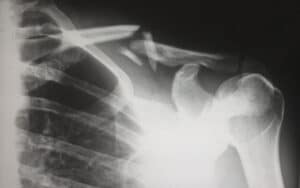
Secondary Osteoporosis
Secondary osteoarthritis happens due to a specific injury or disease. This kind of osteoporosis can happen to younger people due to this factor. There are some factors that can help predispose people to this condition.
· Results of Medication
Some medications can lead to weakened bones and loss of bone density. If you have lost bone density, you might also be more prone to injury. This can lead to a self-fulfilling process of disease processes and injuries that fuel them.
· Results of Diseases
Some diseases can lead to treatments that might cause bone to thin. Cancer and other diseases that require medications that damage bone density can lead to secondary osteoporosis. Bone diseases that are not cancer can also lead to this secondary kind of bone disease.
· Obesity
Being overweight can lead to injury as well other disease processes that can cause you to be predisposed to secondary osteoporosis. Obesity causes a lot of pressure on your overall health and can lead to all kinds of disease processes.
Causes for Osteoporosis
There are some factors that can lead to a predisposition for osteoporosis in everyone, no matter their age.
· Age
Being older than 55 is always a factor when you are considering the development of osteoporosis. Being female is another factor in the development of primary osteoporosis.
· Genetics
Genetic traits can also lead to this disease. If you have irregular bone structures due to improper bone development in childhood or other bone-weakening conditions, you could end up with osteoporosis.
· Nutrition
A poor diet can cause all kinds of health conditions and if you have eaten a poor diet for your whole life, you will find that osteoporosis can be a real risk for your future health. People who suffered from malnutrition, particularly in youth, can have osteoporosis later in life.
· Exercise
Bone density is directly affected by exercising. If you are not using your body for physical activity at least a few times a week, your bones can suffer from weakness and your joints can be negatively impacted by your sedentary lifestyle as well.
· Lifestyle
Being sedentary can put you at major risk for many health conditions. Higher blood pressure, obesity, and weakness in the body can lead to osteoporosis.
· Medications
Some medications can lead to bone loss. If you have to be on pain medications for years or you are taking cancer drugs and other medications that can affect your bones directly, you could end up with osteoporosis.

Signs and Symptoms of Osteoporosis
Osteoporosis can be easily identified in most cases. You will find that age is not the only predictor of this disease process. As a caregiver, you will need to know what the signs of this disease process are so that you can make sure that your patients are safe under your care.
· Bone fractures
Elderly people are not always aware that they have suffered a fracture. This is particularly true of those that are in a lot of pain from other disease processes. You will need to know the signs and symptoms related to fracture to make sure that your elderly patient is not suffering from an injury they are not aware of.
· Kyphosis-Collapsing of the vertebra
A curved spine or a humpback can be a sign of osteoporosis. This can affect all ages of people who have this disease, but you will see it most commonly in those who are older. The breakdown of bone tissue can lead to the spine collapsing and compressing downward on itself, leading to a curved spine or a humped-looking back.
· Decreased calcitonin
This lack of calcium in the blood is most often related to cancer treatment. For those who are undergoing chemotherapy, reduced calcitonin can be a very real concern that can lead to long-term health concerns beyond osteoporosis. This is not usually a reversible process, even in the young.
· Decreased estrogen
Estrogen naturally decreases as women age, but some medication protocols, cancer treatments, and necessary hormone therapies can lead to the progression of osteoporosis-related to this lack of female hormones. If you have been diagnosed with decreased estrogen at a young age, you could face osteoporosis much earlier in life than women who are losing estrogen as a result of aging processes.
· Increased parathyroid hormone
This condition causes calcium levels in your blood to rise too high which can lead to thinning bones and kidney stones. This can be caught early in blood tests, but if it is missed, it can lead to osteoporosis in many people.
Management and Prevention
Prevention and management of this condition often go hand in hand. You want to be sure that you are taking care of preventing further disease processes while also adjusting for management of the condition as it is currently presenting itself.
There are set testing and other kinds of standards that are in place to make sure that men and women who are older and are at risk are tested frequently, but younger people might not get the right attention for this potential disease process unless there is attention to these factors early in their lives.
Diet
Being sure that you are eating correctly to protect against osteoporosis is important and this diet can actually help to treat ongoing osteoporosis as well. Foods that are high in calcium like dairy products, collard greens, kale, okra, tomatoes, sweet potatoes, and spinach can all help to prevent osteoporosis.
You should avoid alcohol, high-salt foods, beans and legumes, wheat bran, large quantities of vitamin A, and caffeine. Eating a balanced diet that is free from fast food and lots of saturated fat can help a lot when combined with avoiding these kinds of unhealthy food items.
Activities and Exercise
Everyone should be exercising at least three times a week for about a half-hour. If your elderly patient cannot do much physical exercise, they can still do gentle exercises that will prevent them from becoming weak and unable to balance. Weight-bearing exercises also lead to increased bone density, even if they are gentle and low-impact.
Lifestyle
Being careful to get enough sleep, eating a good diet, and making sure not to engage in high-risk behavior can help to prevent osteoporosis while also keeping further issues at bay. Lifestyle changes can be very effective toward preventing osteoporosis and can also help manage it when it has already struck.
Fracture Management
Fracture management is a key part of the care of people affected by this disease. Fractures are a daily risk and once they have happened, it can be hard to get them to heal due to the damaged nature of the patient’s bones.
· Medical Management
Medical management of fractures for these people can help to prevent further issues with fractures and keep surgery at bay. These processes include fracture reduction with cast material and non-surgical immobilization. There will also be efforts at physical therapy and rehabilitative exercise for these patients. Anti-osteoporosis therapies can be helpful as well and secondary care for diet and other lifestyle support can all be part of medical management.
· Surgical management
Surgical management is a common solution for these patients since bones with osteoporosis frequently do not heal on their own. This process is delicate, but it can be the only option for people with osteoporosis. The bone is more likely to heal after surgery than it is to heal on its own.
· Fixation
Fixation processes can help to treat osteoporosis fractures. These might be internal in the form of screws and plates, or they could be external devices that are removed after a healing period. These solutions can also be used in concert with one another to treat a difficult fracture or fractures that are in locations that are to stabilize.

Care Plans and Goals for People With Osteoporosis
Caring for people with osteoporosis can be challenging without a proper plan of care. Working with the patient’s doctor or physical therapist can help you to create the right regimen of daily care that will make sure that you can treat their ongoing disease and prevent worsening of their condition.
· Knowledge about osteoporosis treatment regimen
Knowing about the disease itself can help you to prevent issues for your patient and to make sure that you are always thinking about signs and symptoms of further issues that might have cropped up as time passes. You will need to be educated about the common means of treating this condition before you assume that you will be able to create a care plan for an elderly patient that has this disease.
· Relief of pain
Relief of pain for these patients can be tough because they may not be able to have the kinds of pain medications that would manage their pain best. Long—term use of pain medication can lead to further bone damage and can also cause other secondary health problems. Pain management is often about balancing physical therapies with the careful use of pain medications.
· Improved bowel elimination
Straining can be enough to cause fractures in people with osteoporosis. This is part of the diet, but making sure that your patient has no trouble with elimination can help prevent bone issues and fractures related to straining to go to the bathroom. You can support both an improved diet and reduce the risk of a fracture related to bathroom activities.
· Absence of additional fractures
Being able to manage a proper exercise regimen as well as help your patient to move carefully despite ongoing fractures can make it easier to heal existing breaks. You will need to be sure that your patient is not engaging in activities that they should not be doing due to their condition that could lead to further issues.
· Diet
Diet is a key factor in the prevention of osteoporosis as well as a key factor in preventing the progression of this disease. You will need to be sure that you know what diet your patient should be eating for their health and for support of their disease. If you cannot cook for these individuals, there are meal services that can help your patient to eat the right diet reliably enough to improve their disease outlook.
· Exercise
Careful exercise is essential to preventing further breakdown of bone tissue and to help keep the bone density from falling off sharply as your patient becomes more sedentary. You can help your patient to engage in gentle activity that will take care of their need to exercise without being too challenging for their physical condition.
· Lifestyle
Caring for your patient with this disease often includes helping them to make lifestyle adjustments that will keep them healthy even though they are dealing with a bone condition that makes their options limited as far as activity. You will need to be sure that your patient is not exceeding their ability to engage in some activities and that they are being cautious of injury.
· Posture
Slumping and slouching can further the disease processes that lead to curved spine and kyphosis. You need to remind your elderly patient to sit up as much as they can and you should try and prevent any activities that encourage impact to the spine through sloppy or lazy posture. Posture can lead to long-term problems when ignored, and you can help your patient with this disease to avoid a curved spine and other back issues.
· Screenings for Osteoporosis
All people who show any early symptoms of this disease should be screened. All adults 65 and older need to be screened to see if they have the disease and anyone younger than 65 who has genetic or lifestyle indicators for it should be as well.
Fall assessments can also be performed to see if there is a chance that your patient is a fall risk. There are various therapies that your patient can also be assessed for if they are showing early signs of the disease and want to try and ward off its effects on their long-term health.
All of these assessments and screenings can be requested by a patient or by the caregiver acting on their behalf. You will find that some people will be resistant to the screening process and you should encourage them to take their health seriously enough to verify that they do not have this degenerative condition.
Osteoporosis Management Can be Easy With the Right Plan of Care
You will find that having the right care plan in place will make it much easier to take care of your patient that has this disease. If you are caring for someone that has shown early symptoms, you will need to make sure that they consider getting assessed for the disease. Early prevention of this disease is essential to making sure that you can stop the progression in its tracks if possible.
As a caregiver, being able to care for patients with this condition requires attention to detail, willingness to be gentle and thoughtful when helping them with activities, and prevention of fractures and high-risk activities.
