Let’s discuss each Medicaid benefit available to you in NY, with a brief description of what kind of services they include.
Smoking cessation agents
As you already know, smoking can have quite a few harmful effects on your health.
That means long-time smokers are more likely to have more medical needs than non-smokers. Not only is that bad for your health, but it also results in a bigger burden of cost on public health programs like Medicaid.
For these reasons, Medicaid offers smoking cessation agents (professionals who help you quit) to those who want to quit smoking to improve their health and quality of life.
Studies have shown that cessation programs are more effective in helping people quit, and maintain it, than those who try to quit on their own.
With Medicaid cessation, you can expect benefits like nasal spray, nicotine inhaler, and medications. You can also expect individual counseling sessions, and multiple quit attempts per year.

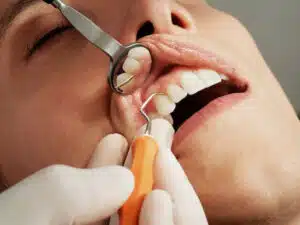
Treatment and preventive health and dental care
Preventing diseases helps you live a better quality of life than if you have to treat a condition after you get sick.
This is why Medicaid is dedicated to providing you access to effective preventative measures like the following.
- Immunizations
- Screenings for chronic diseases, infectious diseases, and cancers
- clinical and behavioral interventions to manage risks of chronic disease
- Health counseling
- Assistance for self-management of chronic disease
For children under 21, Medicaid also offers preventative dental care under the EPSDT plan (more information below). For adults, dental benefits only include very basic services, depending on the insurance provider that handles your Medicaid.
Hospital inpatient and outpatient services
As a Medicaid beneficiary, you will have access to hospital inpatient and outpatient services.
Inpatient services – Inpatient services cover anything that requires you to stay at the hospital for an extended period (including overnight stays). This could include things like surgery, or if you need to spend a few nights to get over an illness.
Outpatient services – This includes anything that doesn’t require you to spend the night at the hospital. For example, if you need to visit the doctor for a consultation. Outpatient also includes visits to the ER, as long as you leave the emergency room on the same day.

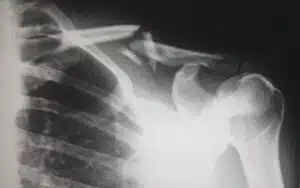
Laboratory tests (including X-Rays)
Lab tests are necessary to diagnose medical conditions so your doctor can then create a treatment plan for you, if necessary.
Here are some of the lab tests that are typically covered in Medicaid plans.
- X-rays
- Routine tests such as pap smears and cholesterol levels
- Ultrasounds
- Mammograms
- Angiograms
- Echocardiograms (ECG)
This is not a comprehensive list. When you sign with a Medicaid provider, be sure to ask about all the tests that are covered under the plan.
Care in a nursing home
If you (or a family member) have a long-term disability that makes it challenging to perform daily living activities at home, then you might consider moving to a long-term care facility, like a nursing home.
The problem is that nursing home costs have been skyrocketing in recent years. Adult day-cares aren’t as pricey as nursing homes, but they definitely aren’t cheap either.
Thankfully, each state, including NY, has Medicaid plans that cover nursing home stays. Your plan will cover basic health services (inpatient, outpatient, etc.) as well as room and board, nursing services, and more, at a nursing home.
Typically, to qualify for a plan that covers nursing home stays, you’d have to prove that you have a disability that prevents you from living a fully functional life at home.

Care through home health agencies and personal care
If you’d prefer not to move to a nursing home, you may also qualify for long-term care at home through CDPAP.
Consumer Directed Personal Assistance Program (CDPAP) is an NY state Medicaid program that allows you to hire your friends and family members as home care providers ((with some exceptions).
You may not want to move to a nursing home for a variety of reasons. Maybe you have privacy concerns, and you don’t want to receive care from a stranger. Perhaps you’re not too keen on the idea of being around other sick people. Or perhaps you want to remain connected to your community.
Whatever your reason might be , CDPAP allows you to receive care at home so you don’t have to move to another facility.
You’ll need to prove that you have a chronic disability that makes it a challenge to perform daily tasks like bathing, grooming, cleaning, meal preparation, and more.
For more information, including how it works and how to apply, be sure to check out our CDPAP page.
Treatment in psychiatric hospitals (for persons under 21 or those 65 and older)
Medicaid covers treatment in psychiatric hospitals for eligible patients under 21 and for those above the age of 65. Plans also include coverage for treatments at mental health facilities and at facilities for those with developmental disabilities.
Your Medicaid plan may also include the following.
- Case management
- Psychiatric evaluation, testing, management, and rehabilitation
- Therapy (individual, group, family)
- Inpatient detoxification
Family planning services
Family planning services promote good health and well-being of the entire family before, during, and after pregnancy.
Regularly visiting doctors, nurses, etc, during the entire process will help make sure that the mother, and the newborn remain in good health.
Family planning also prevents unwanted pregnancies and abortions through education, contraceptives, and more. It allows you to plan your pregnancy when it’s the right time for your family.

Early periodic screening, diagnosis, and treatment for children under 21 (EPSDT)
The Early and Periodic Screening, Diagnostic and Treatment (EPSDT) is a Medicaid feature that covers full preventative services for those under 21 who are enrolled in Medicaid.
It ensures that kids and teenagers get the proper care, whether its mental health, preventative care, dental, developmental care, or other specialty services.
Proper care early in a child’s life is more likely to lead to better outcomes in the future, when it comes to a child’s health, both mental and physical.
Medicine, supplies, medical equipment, and appliances
Medicaid covers any supplies or medicines that you may need, whether it’s to treat an ongoing illness or disability, or its an acute illness.
NY Medicaid plans will cover your prescription drugs. If you need medical supplies, like a wheelchair due to a disability, it will be covered as well.
Clinic services
Clinic services include most of your primary care services. This is where you would go if you’re feeling unwell, if you have a fever, sore throat, a minor injury like a burn or scrape, etc.
Clinic services also include your regular screenings for chronic diseases like diabetes, hypertension, cholesterol levels, and other lab tests.
As we mentioned before, your lab tests are also covered under Medicaid.
Transportation to medical appointments
There are two types of transportation benefits available through Medicaid – emergency and non-emergency.
We’ll cover emergency transport in the section below, but first let’s take a look at non-emergency transport.
Medicaid wants to make sure that you are able to visit your medical provider when you need to see them.
If you have a disability, or your car does not work, or you don’t have a driver’s license, or whatever else might be the reason you can’t get to a doctor on your own, you may be able to arrange transportation, even if it is not a medical emergency.
The specific details of the transportation will depend on a variety of factors. For more information, be sure to ask your provider. You can also visit NY Medicaid’s transportation page for contact information Medicaid transport providers based on your location.

Emergency ambulance transportation to a hospital
When it comes to emergency medical transportation, that is covered by Medicaid as well.
Emergency transportation can be expensive. Since Medicaid is designed for low-income individuals, the plans cover your trip to the ER if you need it.
But your nurse or family members have to make sure that you’re being transported in an emergency vehicle that has been inspected and issued a permit by the state.
Prenatal care
Prenatal care includes all the health services necessary to keep you healthy during pregnancy, to make sure both you and your baby enjoy good health in the long-term.
You get check-ups from your doctors, nurses, midwife, and any necessary other medical service.
If you’re pregnant and uninsured in New York State, you might be eligible to receive medical care through an NY State of Health Marketplace insurance plan. You may be able to sign up even if the enrollment period is closed.
If you lose Medicaid coverage after your pregnancy, you may get extended access to family planning services.
Your baby will also receive health care services for at least one year after birth.
Will I have to pay co-payments?
While Medicaid covers the vast majority of your basic health services, as we discussed above, it doesn’t always cover 100 percent of your expenses.
For some services, you might have to pay a fee out-of-pocket, also known as a co-payment.
When going in to see your doctor, nurse, or other providers, ask them if there is a co-payment involved for the service. If there is, you can pay them directly.
There are some beneficiaries that are always exempt from Medicaid co-pays.
- Children
- Pregnant women
- People who have reached their quarterly limit of Medicaid copay (more details below)
- People who are terminally ill, including those in hospice
- Medicaid recipients who are living in an institution
- Alaska Natives and American Indians who have ever received a treatment from the Indian Health Service, tribal health programs, or under contract health services referral
- Women in the Breast and Cervical Cancer Treatment Medicaid Program are exempt from alternative out of pocket costs
One thing to note is that if your income falls below the federal poverty level, and you’re enrolled in Medicaid, then you can’t be refused medical treatment, even if there is a co-pay. But you might be billed later for any amount you owe.
How do I know if I qualify for Medicaid?
There are some basic requirements to be eligible for Medicaid in New York.
- You must be a resident of the state of New York
- You must be a U.S. citizen, permanent resident, or legal alien
- You must have a medical need that requires you to have health insurance
- Your income must be considered low-income or very low-income
Additionally, you must fall under one of the following categories.
- You’re pregnant
- You’re above 65 years of age
- You (or a family member) has a chronic disability
- You’re diagnosed as blind
- You’re responsible for a child 18 years of age or younger
Since Medicaid is designed for low-income individuals, there are income and resources limits in place in order to qualify, depending on the size of your household.
Visit Benefits.gov for a quiz to determine your eligibility for New York Medicaid.
How do I apply for Medicaid?
Here’s how you can apply for Medicaid in New York.
In-person
Visit your local social services office in NY
Online
You can get the application process started online at the New York State of Health website.
Information
For more information, or if you have any questions, you can visit the NY Medicaid website, or call them at 1-855-355-5777.








